observation of liver cells
Aim
To observe healthy liver cells under compound light microscope
equipment list
- Lamb Liver
- Scalpel
- Probe
- Cover Slip
- Slide
- Cork board
- Microscope
- Dye (Carmin, Eosine, Methyline blue)
method
- Small section of liver was sliced and placed on slide.
- Another slide was placed on top and slides were squeezed together
- Top slide was removed and small amount of liver was taken and placed on another slide
- Small amount of water was dropped on slide and cover slide was placed on top
- 1 drop of dye was placed on top to soak through
- Excess dye was soaked with paper towel
- Steps 1-7 repeated with seperate dye
- Slides were assessed and observed under microscope
risk- Corrosive dye comes into contact with skin or eye
- Slides broken or dropped - Incident with the scapel |
precaution- Wear labcoat and goggles
- Slide is disposed of in the sharps bin and care is used - Teacher present at all times |
Healthy Liver cells

The liver is populated by two types of liver cells; parenchymal cells and non-parenchymal cells. Parenchymal cells, or more commonly known as Hepatocytes, occupy 75-80% of the liver’s cytoplasmic mass. The non-parenchymal cells make up approximately 40% of the total number of liver cells, but only occupy 6.5% of its cytoplasmic mass. Some of the non-parenchymal cells found in the liver are the Sinusoidal Hepatic Endothelial cells, Kupffer cells and Hepatic Stellate cells.
Hepatocytes are involved in Protein synthesis and storage, the transformation of carbohydrates, the synthesis of cholesterol, bile salts and phospholipids, the detoxification, modification and excretion of exogenous and endogenous substances and it also assists initiate the formation and secretion of bile in the liver. In a three dimensional view, hepatocytes are arranged into plates that anastomose with one another. The cells are polygonal in shape and their sides can be in contact either with sinusoids or neighboring hepatocytes . A portion of the lateral faces of hepatocytes is modified to form bile. Microvilli are present abundantly on the sinusoidal face and project sparsely into bile. Hepatocyte nuclei are distinctly round, with one or two prominent nucleoli. A majority of cells have a single nucleus, but binucleate cells are common. The typical hepatocyte has an approximate cubic cell of 15µm sides.
Non-parenchymal cells in the liver participate in the growth of the liver. They assist in the regeneration and repairing of damaged cells within the liver. Majority of the endothelial cells in liver constitute the closed lining or wall of the capillary. The hepatic sinusoid is formed by many different cell types, each with its specific phenotypic characteristics, functions and topography. The main non-parenchymal cells found in the liver are the Kupffer cells, Sinusoidal Hepatic Endothelial cells and Hepatic Stellate cells.
Kupffer cells are one of the main non-parenchymal cells in the liver, as they constitute 80% - 90% of the tissue macrophage in the body. They are located within the lumen of the liver sinusoids, or the capillaries of the liver. Kupffer cells are involved with the liver’s response to infections, toxins, ischemia, resection and other stresses. As they reside within the lumen, Kupffer cells are constantly exposed to gut-derived bacteria, microbial debris and bacterial endotoxins, known to activate macrophages. When Kupffer cells are activated, due to an injury to the liver, they release various products, including cytokines, prostanoides, nitric oxide and reactive oxygen species. The release of these products regulates the phenotypes of the Kupffer cells, and also the phenotypes of it’s neighbouring cells. The neighbouring cells include hepatocytes, stellate cells, endothelial cells and other immune cells that traffic through the liver.
Hepatocytes are involved in Protein synthesis and storage, the transformation of carbohydrates, the synthesis of cholesterol, bile salts and phospholipids, the detoxification, modification and excretion of exogenous and endogenous substances and it also assists initiate the formation and secretion of bile in the liver. In a three dimensional view, hepatocytes are arranged into plates that anastomose with one another. The cells are polygonal in shape and their sides can be in contact either with sinusoids or neighboring hepatocytes . A portion of the lateral faces of hepatocytes is modified to form bile. Microvilli are present abundantly on the sinusoidal face and project sparsely into bile. Hepatocyte nuclei are distinctly round, with one or two prominent nucleoli. A majority of cells have a single nucleus, but binucleate cells are common. The typical hepatocyte has an approximate cubic cell of 15µm sides.
Non-parenchymal cells in the liver participate in the growth of the liver. They assist in the regeneration and repairing of damaged cells within the liver. Majority of the endothelial cells in liver constitute the closed lining or wall of the capillary. The hepatic sinusoid is formed by many different cell types, each with its specific phenotypic characteristics, functions and topography. The main non-parenchymal cells found in the liver are the Kupffer cells, Sinusoidal Hepatic Endothelial cells and Hepatic Stellate cells.
Kupffer cells are one of the main non-parenchymal cells in the liver, as they constitute 80% - 90% of the tissue macrophage in the body. They are located within the lumen of the liver sinusoids, or the capillaries of the liver. Kupffer cells are involved with the liver’s response to infections, toxins, ischemia, resection and other stresses. As they reside within the lumen, Kupffer cells are constantly exposed to gut-derived bacteria, microbial debris and bacterial endotoxins, known to activate macrophages. When Kupffer cells are activated, due to an injury to the liver, they release various products, including cytokines, prostanoides, nitric oxide and reactive oxygen species. The release of these products regulates the phenotypes of the Kupffer cells, and also the phenotypes of it’s neighbouring cells. The neighbouring cells include hepatocytes, stellate cells, endothelial cells and other immune cells that traffic through the liver.
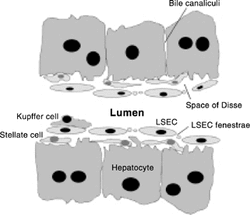
The liver has endothelial cells, which form a continuous lining of the liver capillaries, or sinusoids, separating parenchymal cells and fat-storing cells from sinusoidal blood. The difference between liver endothelial cells and liver sinusoidal endothelial cells is that the structure of the sinusoidal endothelial cell lack a distinct basement membrane and also contain open pores, or fenestrae, in the thin cytoplasmic projections which constitute the sinusoidal wall. This change and morphology in the cells supports the protective role played by the liver endothelium, where the cells form a general barrier against pathogenic agents and assist as a selective sieve for substances passing from the blood to parenchymal and fat-storing cells. They have been shown to be involved in the endocytosis and metabolism of a wide range of macromolecules, including glycoproteins, lipoproteins and establishing endothelial cells as a vital link in the complex network of cellular interactions and cooperation in the liver. Overall, sinusoidal endothelial cells significantly participate in the metabolic and clearance functions of the liver.
Hepatic Stellate cells are very important non-parenchymal cells in the liver, as they are the main-matrix producing cells in the process of liver fibrosis. They are located in the Space of Disse and preserve close interactions with the sinusoidal endothelial cells and the hepatic epithelial cells. Much research has now shown that hepatic stellate cells have a profound impact on the differentiation, proliferation, and morphogenesis of other hepatic cell types during liver development and regeneration. Any form of injury to the liver will ultimately lead to the activation of the Hepatic Stellate cells, which undergo transdifferentiation to fibrogenic myofibroblast-like cells. In the regeneration process, Hepatic Stellate cells express specific receptors for retinol-binding protein, a binding protein specific for retinol, on their surface, and take up the complex of retinol and retinol-binding protein by receptor-mediated endocytosis. Furthermore, Hepatic Stellate Cells are involved with the development and regeneration process of the liver through the activation of the Stellate Cells and triggering the liver fibrogenesis.
The liver consists of parenchymal, or hepatocytes, and various forms of non-parenchymal cells. The Hepatocytes assist with the livers general function, for example protein synthesis and storage, transformation of carbohydrates, etc. Whereas, the non-parenchymal cells, such as Kupffer cells, Sinusoidal Hepatic Endothelial cells and Hepatic Stellate cells, are involved in the regeneration, detoxification and healing of an injured liver.
Hepatic Stellate cells are very important non-parenchymal cells in the liver, as they are the main-matrix producing cells in the process of liver fibrosis. They are located in the Space of Disse and preserve close interactions with the sinusoidal endothelial cells and the hepatic epithelial cells. Much research has now shown that hepatic stellate cells have a profound impact on the differentiation, proliferation, and morphogenesis of other hepatic cell types during liver development and regeneration. Any form of injury to the liver will ultimately lead to the activation of the Hepatic Stellate cells, which undergo transdifferentiation to fibrogenic myofibroblast-like cells. In the regeneration process, Hepatic Stellate cells express specific receptors for retinol-binding protein, a binding protein specific for retinol, on their surface, and take up the complex of retinol and retinol-binding protein by receptor-mediated endocytosis. Furthermore, Hepatic Stellate Cells are involved with the development and regeneration process of the liver through the activation of the Stellate Cells and triggering the liver fibrogenesis.
The liver consists of parenchymal, or hepatocytes, and various forms of non-parenchymal cells. The Hepatocytes assist with the livers general function, for example protein synthesis and storage, transformation of carbohydrates, etc. Whereas, the non-parenchymal cells, such as Kupffer cells, Sinusoidal Hepatic Endothelial cells and Hepatic Stellate cells, are involved in the regeneration, detoxification and healing of an injured liver.
unhealthy liver cells

As described in stunning detail above, Hepatocytes are incredibly important to the liver. They do a huge amount of work, and it’s a disaster if they shut down. There are eight different kinds of hepatocellular disease, all of which have differing mechanisms of toxicity, and most of which are congenital (like Wilson’s Disease) or largely self-inflicted (like alcohol poisoning). There are, however, plenty which can be inflicted, falling under the categories of infections and drugs and toxins.

A Virus (such as Viral Hepatitis) will invade the cell and change the structure of the DNA within, and can be deliberately transferred through infected needles, or anything else which will make contact with the bloodstream.
Viruses which affect the liver are generally hepatocellular, which, as its name suggests, denotes an injury to the hepatocytes which leads to decreased metabolic activity and release of intracellular contents (ALanine-amino Transferase, an enzyme which participates in modifying amino acids, and ASpartate aminoTransferase). The injury is, predictably, to the hepatocytes, and we test for it by looking for abnormalities in AST/ALT and PT/albumin commonly referred to as HEPATITIS, and it looks like this:
Viruses which affect the liver are generally hepatocellular, which, as its name suggests, denotes an injury to the hepatocytes which leads to decreased metabolic activity and release of intracellular contents (ALanine-amino Transferase, an enzyme which participates in modifying amino acids, and ASpartate aminoTransferase). The injury is, predictably, to the hepatocytes, and we test for it by looking for abnormalities in AST/ALT and PT/albumin commonly referred to as HEPATITIS, and it looks like this:

The duration of the illness affects the hepatic cells differently; acute hepatitis is different from chronic hepatitis

Acute Hepatitis
A new liver disease, which will usually heal completely because the liver is amazing and its cells regenerate very quickly, and lasts less than 2-3 months, generally.
Chronic Hepatitis
A persistent liver disease, continuing for more than 6 months, and may evolve through fibrosis to cirrhosis or hepatocellular carcinoma.
Your liver function is determined by the number of functional hepatocytes - determined by the sum of:
A new liver disease, which will usually heal completely because the liver is amazing and its cells regenerate very quickly, and lasts less than 2-3 months, generally.
Chronic Hepatitis
A persistent liver disease, continuing for more than 6 months, and may evolve through fibrosis to cirrhosis or hepatocellular carcinoma.
Your liver function is determined by the number of functional hepatocytes - determined by the sum of:
- Hepatocyte dysfunction
- Hepatocyte death rate
- Duration of disease
- Regeneration rate
It must be noted that, just like with every organ, the phrase “impaired function” DOES NOT mean that it no longer works. You can survive for quite a long time if one of your organs has impaired function, and there are a few poisons that affect both the heart and the liver, and it is entirely possible for your heart to outlast your liver if you had been subjected to a poison which affects both. The phrase to look for is “liver failure” which describes the situation wherein the liver cells are destroyed faster than the liver can replace them until the liver shuts down.

There is also cholestasis to worry about. Cholestasis is impaired bile formation (through hepatocytes) or impaired bile flow (through bile ducts or ductules) which leads to a build-up of gunk in the blood stream which would normally have been removed or excreted through the bile (bilirubin, or bile acids), and the release of apical membrane proteins (the Apical membrane being the microvilli-bearing portion of the epithelial cell membrane at the secretory pole)
Hepatocellular cholestasis is most commonly caused by cirrhosis and drug reactions, but there are plenty of others such as Viral Hepatitis, Alpha-1-Antitrypsin Deficiency, and assorted congenital disorders, syndromes, etc.
Hepatocellular cholestasis is most commonly caused by cirrhosis and drug reactions, but there are plenty of others such as Viral Hepatitis, Alpha-1-Antitrypsin Deficiency, and assorted congenital disorders, syndromes, etc.
